Checking a patient’s eligibility to receive services from an agency is essential to providing care. Navigate to the Eligibility tab in Axxess RCM to check eligibility and view details for existing eligibility requests.

Search for eligibility requests by entering the provider NPI, patient name, or payer. The tab provides details of the time of request, patient name/subscriber ID, payer, provider, status of the request, and request reference ID.
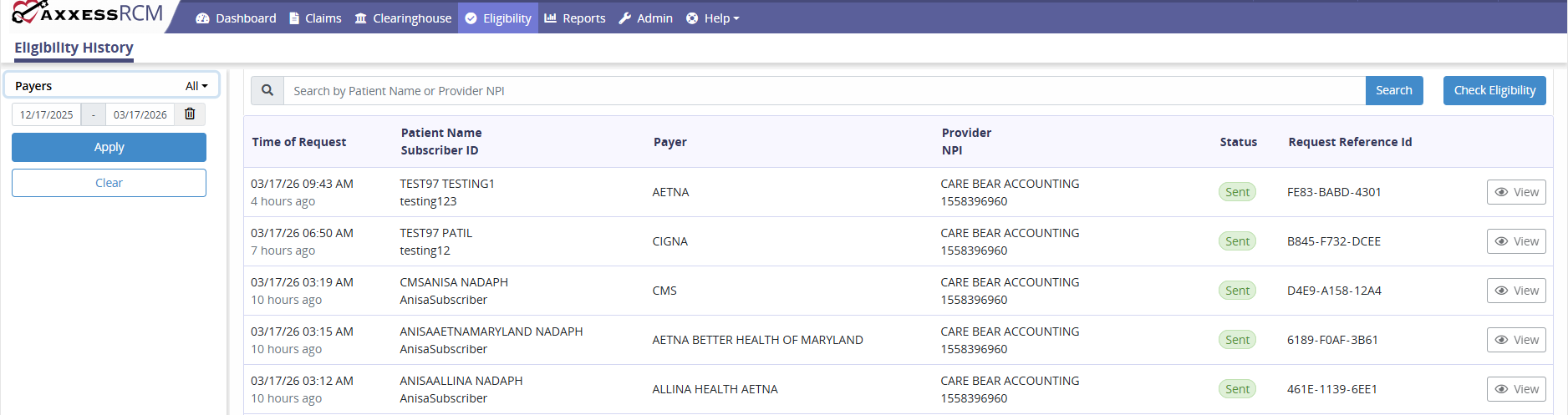
Select the Check Eligibility button at the top of the screen to expand the below form. Enter the payer, provider, date range of service, patient first name, patient last name, patient date of birth, patient gender, subscriber ID, and patient relationship to subscriber, and click on Submit.
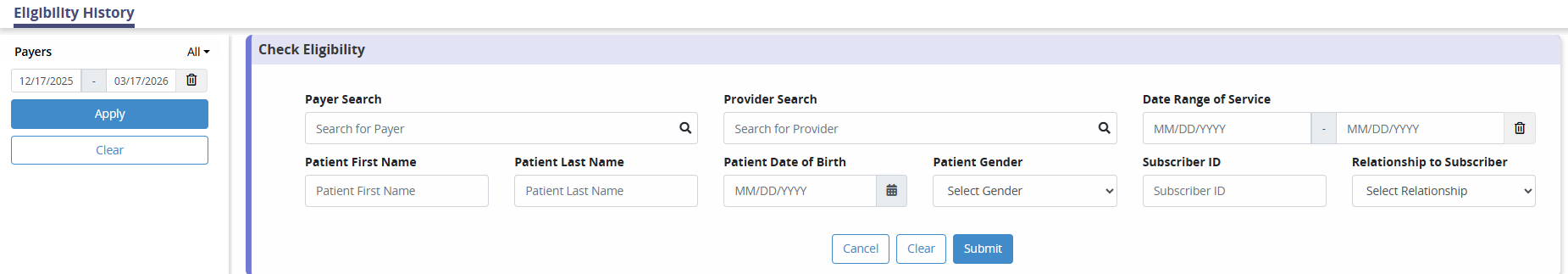
To generate a patient’s eligibility details, all sections must be completed. Eligibility data will appear within 24 hours of the request.