Axxess RCM’s landing page is the Dashboard. It displays the following widgets: Top 10 Error Reason Codes, Electronic Remittance Advice (ERA), Pass Rate, Ready to Work Items, Edit/Error Management Aging, Submissions, and News and Updates.

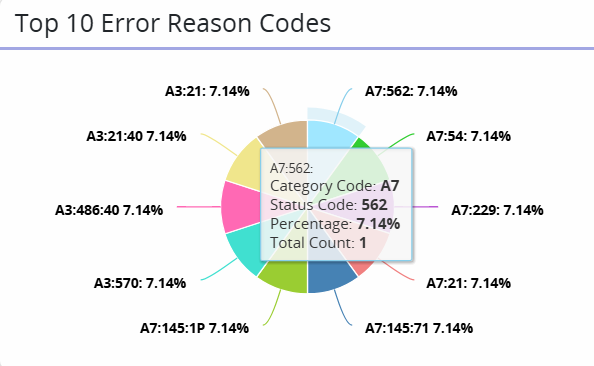
The Top 10 Error Reason Codes widget displays the 10 most frequently used error reason codes in a pie chart. Hover over the pie chart to display the following details:
Category Code: The general classification of claim statuses.
Status Code: A two-digit code that represents the status of the claim.
Percentage: The percentage each reason code has occurred in relation to the total sum of claims.
Total Count: The sum of claims with the specified reason code.
Click anywhere on the pie chart to open the Top 10 Error Reason Codes Report.
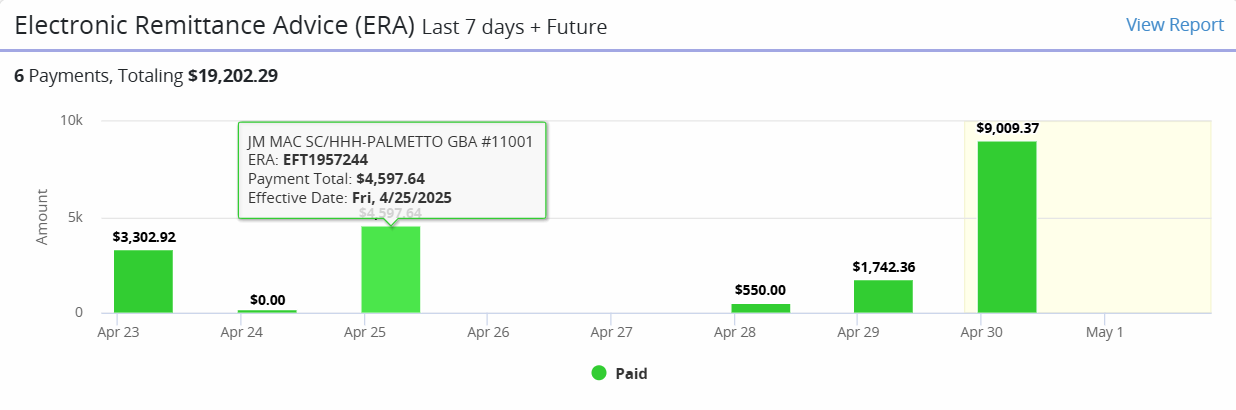
The Electronic Remittance Advice (ERA) widget displays the organization’s checks in a bar graph for the previous seven days and future dates. Hover over the bar graph to see payment details, including the payer, EFT number, amount, and date. Click anywhere on the bar graph to open the Remittance Details screen.
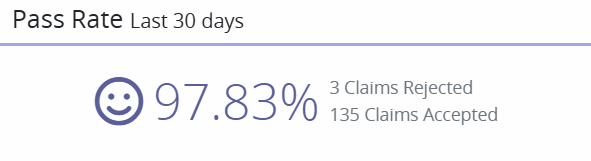
The Pass Rate widget displays the percent of claims that were accepted by the payer. The smiley face icon adjusts based on the pass rate.
The Ready to Work Items widget displays the number of claims that have errors, were denied, or were not submitted. Click on a section to open and work those claims.
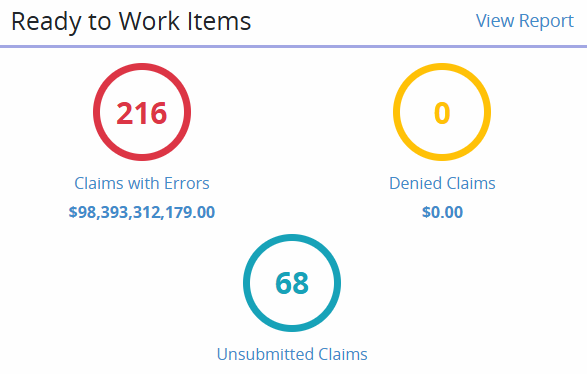
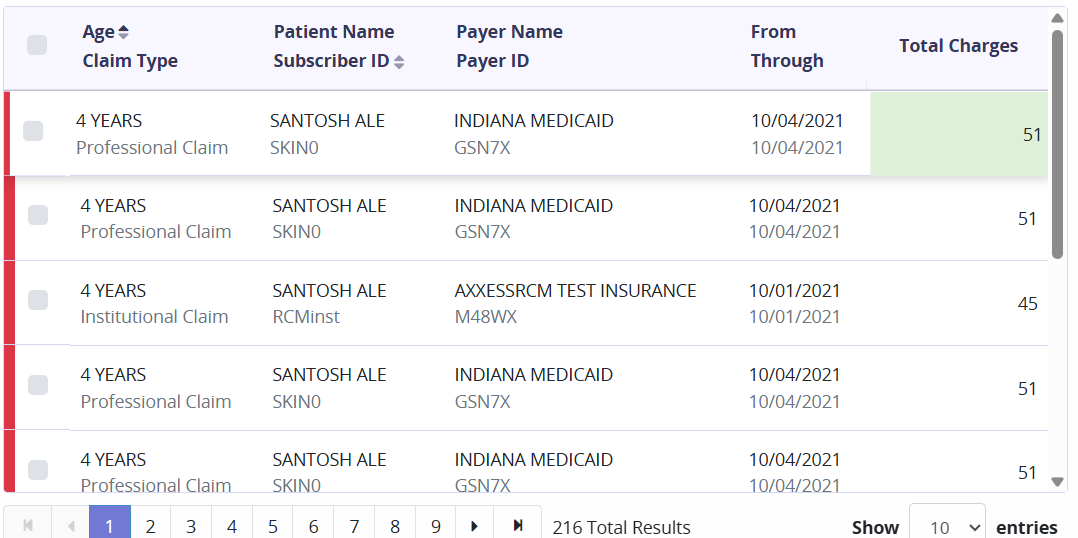
When Claims with Errors is selected, all claims with errors, whether validation errors or payer rejection errors, will appear on the Ready to Work screen. Select the desired claim to view its details.
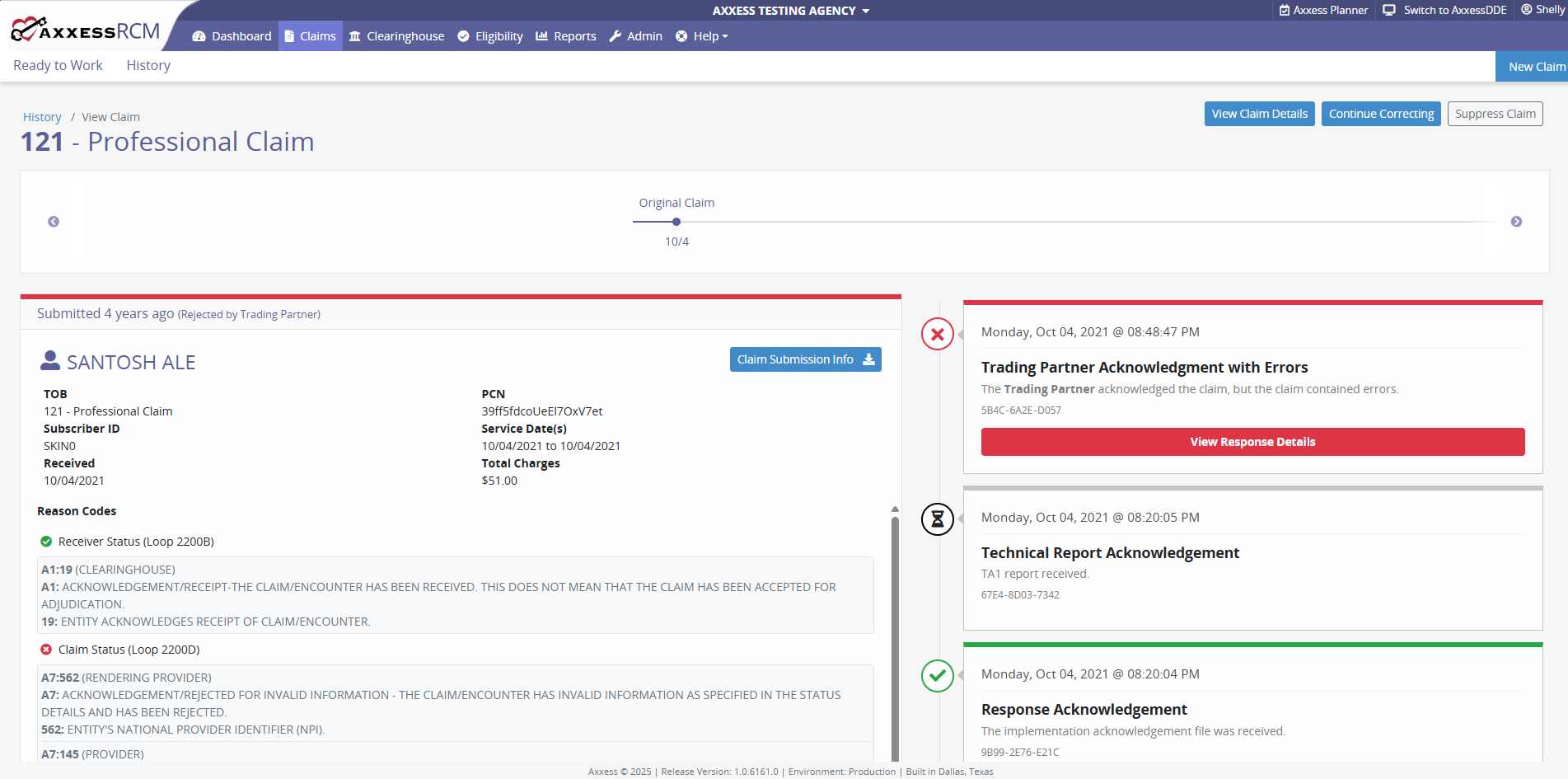
Click View Claim, View Claim Details, Continue Correcting, or Suppress Claim in the top-right corner of the screen.

View Claim displays the claim’s history (submission, acknowledgement, validation errors, error information).
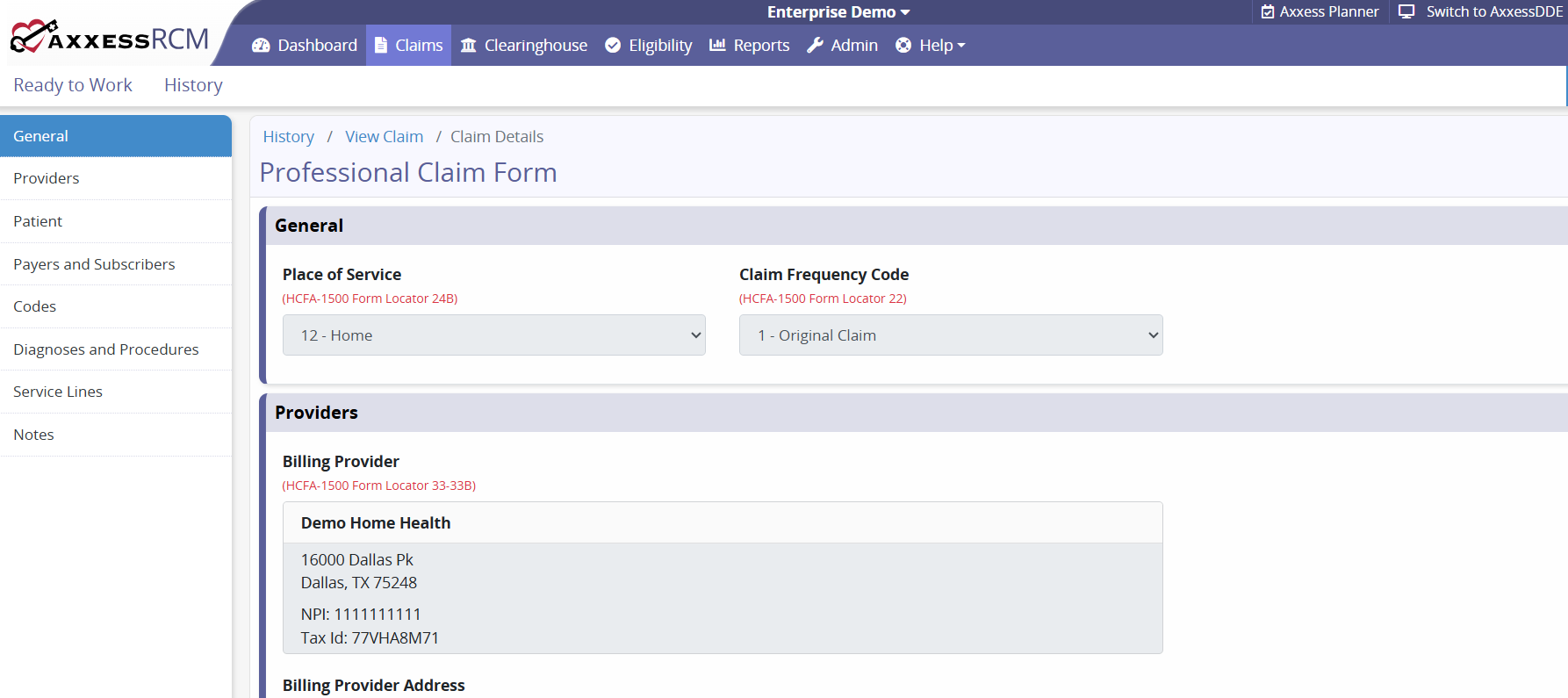
View Claim Details opens the claim to display its details and enables the user to start editing/correcting the claim.
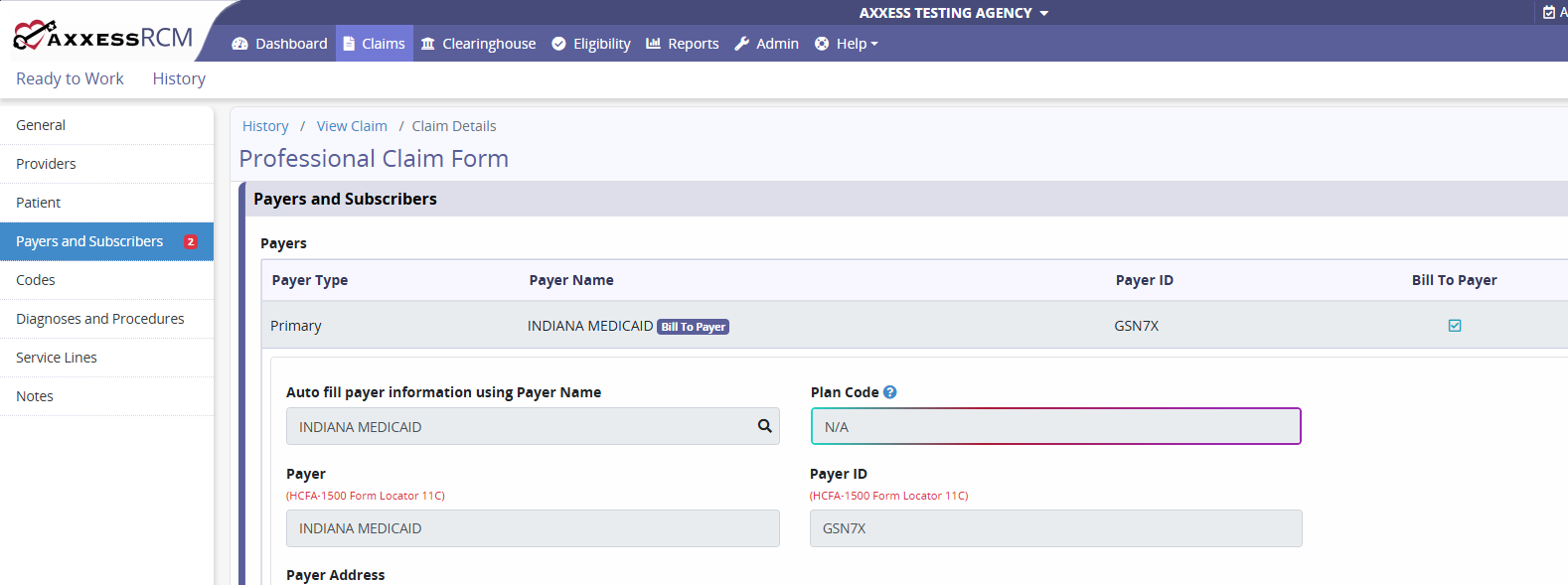
Correct Claim/Continue Correcting opens the claim to allow for correcting.
Suppress Claim removes the claim from the Ready to Work screen.
Once the necessary corrections have been made, click Submit Claim, Save Claim, Validate Claim, View Response or Cancel.
When Denied Claims is selected from the Ready to Work Items widget on the Dashboard, the Ready to Work screen will open and display all denied claims. Select the desired claim to view its details.
When Unsubmitted Claims is selected from the Ready to Work Items widget on the Dashboard, the Ready to Work screen will open and display all unsubmitted claims. Select the desired claim to view its details.
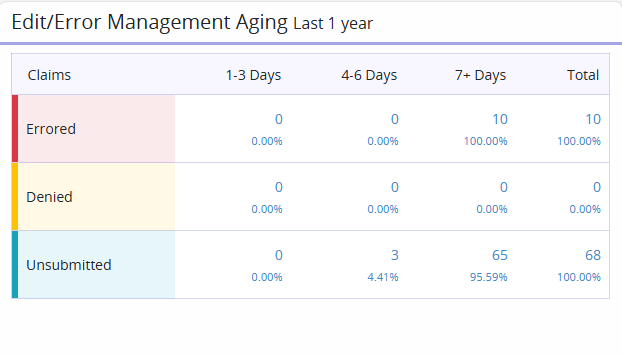
The Edit/Error Management Aging widget displays claim statuses categorized into aging buckets. Totals of each claim status appear in the last column.
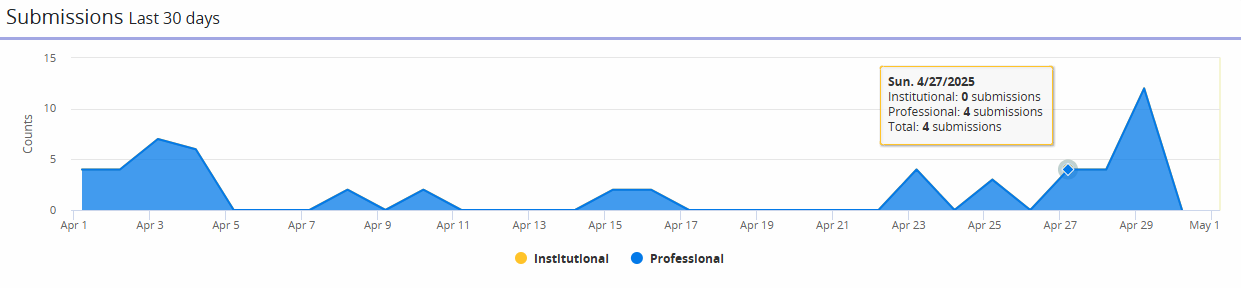
The Submissions widget provides a line graph with the total count of submitted claims within the previous 30 days. Hover over the graph to see how many submitted claims were institutional versus professional. Click on the Professional and Institutional items in the legend to indicate which claim types to display on the graph.
The News and Updates widget provides direct links to Axxess blog posts, educational articles, regulatory updates and other important information to help your organization succeed.
