
The Home Health Value-Based Purchasing (HHVBP) Model was designed by the Centers for Medicare and Medicaid Services (CMS) to incentivize the delivery of high-quality, cost-effective home healthcare. Under the HHVBP Model, CMS evaluates home healthcare organizations’ performance on a set of specific quality measures and allocates reimbursement based on each organization’s scoring, relative to their peers’ scoring, incentivizing the quality rather than the quantity of care.
In an education session at the 2023 Axxess Growth, Innovation and Leadership Experience (AGILE), Lisa McClammy, BSN, RN, COS-C, HCS-D, HCS-O, Senior Clinical Education Consultant at MAC Legacy, and Mike Carr, PT, COS-C, Senior Product Manager at Axxess, broke down the three categories used to calculate VBP scoring and provided actionable strategies to optimize VBP performance and sustain lasting financial health.
The Value-Based Purchasing Triathlon
The VBP scoring measures fall into three overarching categories, which can be conceptualized as a triathlon, where scoring for each distinct part is combined to generate one final score:
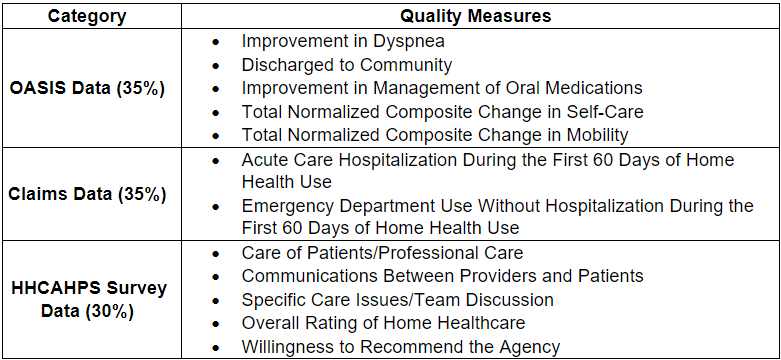
Monitoring these measures is essential to optimizing VBP performance and protecting and increasing reimbursement.
Winning Strategies for VBP
Carr and McClammy outlined the following strategies for VBP success:
Data Analysis and Performance Improvement
The first step to improving VBP performance is identifying where the organization stands currently on each performance measure.
“You’ve got to know what your data is,” McClammy said. “To me, the low-hanging fruit are the first things.” She encouraged organizations to review their data and identify areas that can be immediately targeted for improvement.
Both Carr and McClammy emphasized the importance of access to real-time data, discouraging organizations from relying exclusively on Care Compare where publicly reported data is delayed. “You need something in your EMR or an interface with a vendor that supplies that real-time [data],” Carr said. Access to real-time data is critical for continuous data monitoring and timely improvement targeting.
Areas that require improvement can be targeted through a performance improvement (PI) project. “If you’re identifying a problem or a trend and you can fix it through a PI project, make it fun,” McClammy said. “Get everybody’s input. Everybody probably has input on how they can improve a score. Find out what that is.”
OASIS Accuracy
“[OASIS accuracy] is one of the biggest areas [where] you can make improvement without having to spend a lot of resources,” McClammy said. “Your clinicians want to do the right thing. They want to answer those questions correctly.”
She encouraged organizations to train and retrain clinicians on the following critical elements:
- Score before you fix: “Make sure [clinicians are] scoring [patients] how they found them,” McClammy said. “Then when you come back and reassess, you’ve made improvements…Make sure they understand that, because sometimes they’ll fix [a problem] while they’re there and then they’ll score based on the fix. You don’t want to do that.”
- Think of the OASIS as a walk, not an interview: “If you don’t walk your patient to every one of [their] rooms, you haven’t done a full assessment,” McClammy said. “You can’t know how they get in and out of the bed if you don’t go to the bed.”
- Collaborate: Collaborate with every staff member who has contact with the patient, including therapists and aides. “[The] OASIS doesn’t need to be done in a day,” Carr said. “We have that five-day window. If you’re not using it, you’re missing an opportunity to share minds…[to] get the right answer. The right answer isn’t always the nurse answer being two or the therapist answer being three. It needs to be discussed to see which [is] the more correct answer.”
Prevent Hospitalizations
Hospitalizations comprise 26% of an organization’s total VBP score. “Of all the individual items, that’s the one to focus on the most,” Carr said. “If you don’t do anything else well, focus on keeping your patients out of the hospital because that’s your biggest margin for improvement.”
Carr and McClammy identified falls and medication issues as the two most common reasons for hospitalizations. To minimize hospitalizations, organizations must focus on preventing falls and managing medications and diseases appropriately.
“Make sure that those interventions are patient-specific,” McClammy said. “That patient may have stairs that they have to access. They may have a step up or down to get into their living room…so make sure that…your interventions and goals based on your fall prevention program are specific to that patient.”
Other ways to prevent hospitalizations include maintaining an interdisciplinary team approach, scheduling telehealth visits between in-person visits, front-loading visits and staggering disciplines.
Patient Engagement
The third broad category included in VBP scoring is HHCAHPS Survey results. Implement the following best practices to improve HHCAHPS Survey performance:
- Provide all staff with the HHCAHPS Survey questions.
- Inform patients during admission that they may receive a survey.
- Use key phrases (scripting) when interacting with patients.
- Track all patient calls and follow until resolved.
- Investigate every complaint and incident.
For additional information on how to improve HHCAHPS Survey scores, read this Axxess blog.
“The nice opportunity about value-based purchasing is there’ll be agencies that succeed and do very well,” Carr said. “The potential is there…to have an increased revenue…so whether you’re a great elite marathoner or whether you’re just getting better than where you were, there’s still opportunity for success.”
With more than 250 attendees, more than 40 sponsors and countless connections made, AGILE 2023 was a massive success for everyone. Check out the recap video and register now for AGILE 2024, April 21-24 in Dallas.
