
The Consumer Assessment of Healthcare Providers and Systems (CAHPS) Hospice Survey empowers hospice organizations by attracting referral sources, driving business growth, and sustaining compliance with industry regulations, including the current pay-for-reporting requirements and the shift to value-based care on the industry’s horizon. By evaluating hospice patient and caregiver experiences, the CAHPS Hospice Survey delivers valuable insights to hospice organizations and contributes to ongoing efforts to improve patient and family experiences. Understanding the impact of the CAHPS Hospice Survey and how to improve ratings is essential to hospices’ long-term growth and sustainability.
Question 10 – Avoiding Confusing and Contradictory Information
Question 10 is one of six questions comprising the Communication with Family domain, designed to assess the hospice team’s communication proficiency.
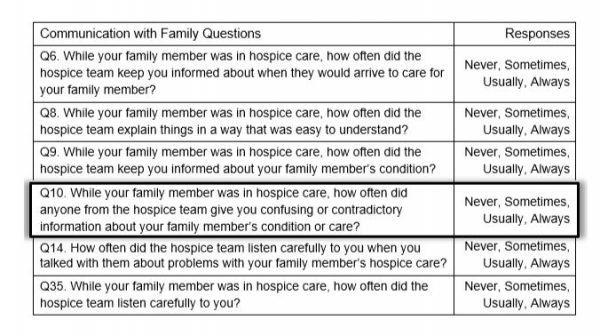
This question evaluates the caregiver’s perception of how frequently members of the hospice interdisciplinary team provided confusing or contradictory information when discussing the patient’s condition or care. Optimizing performance on this question relies on the abilities of hospice providers to communicate clearly and work collaboratively so all members of the interdisciplinary team provide unified, consistent information.
Tips to Improve Communication with Patients and Families
- When speaking with patients and family caregivers, use plain language that is specific and direct. Avoid euphemisms to prevent ambiguity and misinterpretation. Passing on and passing away are ambiguous. Dying is direct.
- Accommodate individual communication needs of patients and family members, including primary language, health literacy proficiency and individual preferences, to avoid confusion.
- Emphasize the importance of care continuity in all business operations and maintain an expectation that all staff adhere to established procedures to deliver consistent communication throughout care.
- Promote an organizational culture rooted in collaboration where staff members operate as a team and communicate productively with each other to deliver exceptional patient and family experiences.
Receiving confusing or conflicting information from healthcare providers can be unsettling during an already challenging time for many hospice patients and their families. It is imperative that hospice providers continuously work toward communication competency to facilitate productive transactions and equip patients and family caregivers with appropriate information to manage their roles in hospice care effectively.
Providing consistent information across providers and throughout the care continuum requires concerted efforts from all members of the hospice interdisciplinary team. Implement the following best practices to achieve optimal performance on this survey question and deliver the best possible care experience.
Best Practices for Collaborative Communication
- Use consistent terminology. All members of the IDG team should use consistent language when communicating with care recipients and when speaking internally with each other. If one member of the hospice team says a patient is transitioning and another staff member says the patient is becoming imminent, seemingly interchangeable terms to hospice professionals can be perceived by patients and families as inconsistent or unclear information. Establish companywide standards for frequently used terminology and review them during staff onboarding and regular IDG meetings to facilitate adherence to the instituted terms.
- Use plain language that accommodates low health literacy. The Agency for Healthcare Research and Quality (AHRQ) provides a health literacy toolkit with a list of commonly used complex healthcare terms and corresponding plain language alternatives that care recipients can readily understand. Examples include joint pain as an alternative to arthritis and high blood pressure as an alternative to hypertension. Encouraging healthcare providers to brainstorm plain language alternatives for complex medical terms is a good exercise to continually sharpen communication adeptness and nurture teambuilding.
- Train staff to discuss difficult topics clearly and proficiently. People often intersperse euphemisms when discussing difficult subjects like death and serious illness. Healthcare professionals should avoid euphemisms, which can dilute clinical accuracy and cause misunderstanding. Train providers to consistently use explicit, direct terms and be familiar with confronting difficult topics skillfully without introducing clinical ambiguity. Hospice providers should be well-accustomed to addressing challenging topics and discussing death in a manner that is both comforting to care recipients while remaining straightforward and clear.
- Leverage technology to streamline processes. Maintain thorough and compliant documentation in a hospice software and train all staff to use the software to its fullest capacity. Capitalize on collaboration tools and features in the software system, including using comments and note sections to record important information about the patient’s condition and care. Reference this information during IDG reviews and train staff to refresh themselves on important details before communicating with patients and family members.
- Establish and adhere to company-wide processes that promote team cohesion. Exercise company-wide expectations and protocols that promote collaboration among IDG team members, and employ technology and resources to develop your interdisciplinary groups and sustain team cohesion. All quality improvement efforts should remain deeply entrenched in team collaboration and optimal care delivery as a common, persistent objective.
Check our blogs for the series on improving CAHPS Hospice Survey scores by systematically reviewing each survey question and exploring opportunities for improvement. Our next installment will continue the discussion on optimizing communication between hospice care providers and recipients to improve the quality of patient and family lives.
