
The Norton Pressure Ulcer Risk-Assessment Scale is a tool designed to help clinicians evaluate patients’ risk of developing pressure injuries. Nurse Doreen Norton developed the scale in 1962 and it has been widely used since its creation. Today, it is one of the three most-used tools and is comparable in predictive validity to the Braden Scale and the Waterlow Pressure Area Risk Assessment.
The five components of the Norton Scale encompass a large portion of the comprehensive assessment and Outcome and Assessment Information Set (OASIS) items to help determine the risk for a pressure injury. A score greater than 18 indicates low risk, between 18 and 14 indicates medium risk and between 13 and 10 indicates high risk. A score less than 10 indicates very high risk.
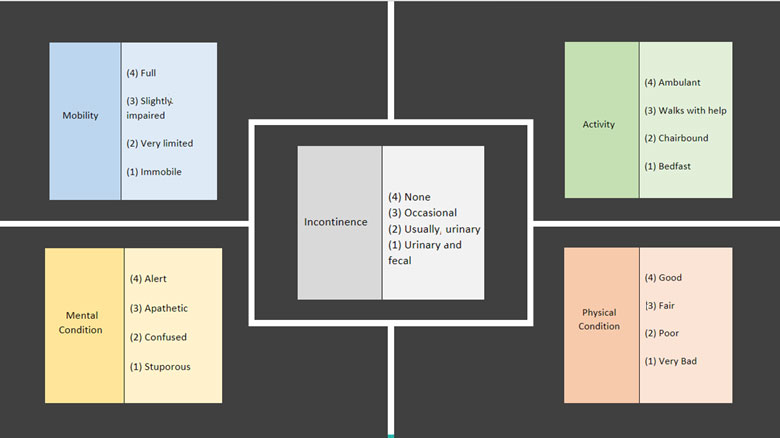

To complete the scale, clinicians should review OASIS and comprehensive assessment findings to score the parameters. The following gives an overview of each part of the scale and areas of the comprehensive assessment and OASIS questions to consider.
Physical Condition generally considers dysfunctions, injuries or illnesses, not including mental illness or substance abuse. This parameter may be scored as good, fair, poor or very bad.
- M1021 and M1023: How many diagnoses does the patient have and how severe are they?
- O0110: Is the patient receiving any special treatments, which may include chemotherapy, oxygen, IV medication or dialysis?
- What is the patient’s prognosis?
- How did this patient score on hospitalization and infection risk?
- Are there recent abnormal lab results or an ongoing infection?
- Is the body mass index (BMI) much lower or higher than the normal range?
Mental Condition is the capacity of thinking, decision-making, behavior or mood. Scoring options are alert, apathetic, confused or stuporous.
- BIMS score: Are they alert and oriented to their situation and do they understand the need to reduce pressure ulcer risk?
- PHQ-2 to 9: Is the patient depressed or apathetic toward self-care?
- Are they taking multiple medications to treat anxiety, depression or psychosis that may indicate the inability to recognize a sign of a pressure ulcer?
Activity measures the patient’s ability to walk and considers the level of activity with ambulant, walks with help, chairbound or bedfast.
- Sensory status: If the patient is unable to see clearly, are they avoiding ambulating?
- Pain status: If pain is not controlled, the patient may rely on assistance or a wheelchair.
- Functional abilities and goals: Do they have physical therapy or an aide ordered or recommended?
Mobility measures a patient’s ability to move themselves from full, slightly impaired, very limited or immobile. This is a good time to collaborate with the physical and occupational therapists.
- Functional status: Consider the functional assessment, such as whether the patient is able to move their body in a way to off-load their pressure points without assistance.
- Supportive assistance: Do they have help to change positions or transfer, if needed?
Incontinence, a major contributor to pressure ulcer risk, is scored none, occasional, usually urinary or urinary and fecal.
- Genitourinary assessment: The level of urinary incontinence and concentration of urine or signs of infection greatly increase the risk of skin breakdown from the surface.
- Gastrointestinal assessment: What’s the level of fecal incontinence and type of bowel movement?
- M1600-1630: Does the patient have an ostomy for bowel elimination that may reduce the risk of breakdown over bony prominences?
In Axxess solutions, the score is automatically calculated as clinicians make selections on the scale. When scoring the scale, clinicians must consider their assessment and the impact of their findings on the ability to relieve pressure to the areas of risk. When the Norton Scale score is low and the patient is found with deficits, an intervention is needed to mitigate the risk. The Norton Scale is a helpful tool to assist clinicians in evaluating and individualizing the care plan for a particular patient.
Looking to further develop your clinical leadership skills? The Axxess Growth, Innovation and Leadership Experience, known as AGILE, will bring together the brightest thought leaders, policymakers, technology innovators and care teams to envision a shared future of healthcare at home. It’s more than just a user conference. Save your spot today.
