
Home health providers will need to adapt to a lot of changes when the Patient-Driven Groupings Model (PDGM) begins in January 2020. One of the most significant changes CMS has made in the new payment model is the threshold for a Low Utilization Payment Adjustment, or LUPA. Under PDGM, billing occurs on a 30-day payment period instead of the current 60-day period. The shorter period for payments means the threshold for a reaching a LUPA also changes, but there is more to the change than simply cutting the number of acceptable visits in half.
Changing from PPS to PDGM
PDGM continues the practice of counting all billable visits toward the episode reimbursement threshold. Episodes that fall under the LUPA threshold are not reimbursed in the same way as a standard episode. Rather than reimbursing a fixed amount, the LUPA episode is reimbursed on a ‘per-visit’ basis. According to CMS, the CY2019 per-visit rate for providers that submit quality reporting data is as follows:
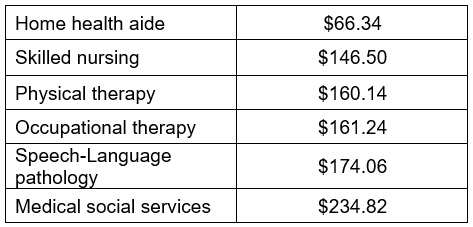
The bottom line with these LUPA payments is that even under PDGM they are substantially less than the full episode payment.
How a LUPA is Caused
There are many different factors that can cause a LUPA to occur. An expected LUPA occurs when an agency admits and understands that a particular patient will not require enough visits to exceed the LUPA threshold. An example of this would be a patient who requires a Foley catheter change only once every 30 days. Barring any unforeseen circumstances, an administrator should expect that patient to result in a LUPA. An example of a non-avoidable LUPA is when a patient refuses any further care, or is readmitted to an acute care facility and never returns to the agency’s care.
Avoiding a LUPA
Sometimes LUPAs can be avoided altogether by retraining agency staff. There’s one example that stands out for me; I had a nurse who was scheduled to see a patient on a Friday, but when she got to the patient’s home no one was there. Rather than call me at the office to report the missed visit, the nurse called the doctor’s office and discovered the patient was at a pre-scheduled appointment. If the nurse had called me in the office, we could have rescheduled our visit to the next day and avoided a LUPA.
Under PDGM, referrals from institutions are paid at a higher rate than community-based referrals, so there is an incentive to accept patients from acute care facilities. Patients often require frontloading of visits at the beginning of an episode to prevent repeat hospitalizations. Often visits are tapered during the second 30-day period. The important thing for administrators and staff to know is that by tapering a visit in the second 30 days, the organization could be setting itself up for a LUPA under PDGM.
The new PDGM system is designed to allocate resources correctly to the population groups that historically require the most resources. It is natural for the new model to also incorporate a new reimbursement methodology to include LUPAs.
PDGM Success with Axxess
Axxess is a partner helping providers on the journey to PDGM success. We have created a wide variety of resources to help providers understand the new regulations, including on-demand webinars, web articles, and quick reference guides. We are also incorporating features into our software to help our clients understand the impact of PDGM on the clinical, operational, and financial process and provide suggestions for improvement.

